Bruxism, Masseter Hypertrophy, and Botulinum Toxin: A Comprehensive Review
Postgraduate Level
Equivalence to 1 CPD/CME point — we do not award CPD/CME directly
Read the article, complete a short assessment, and submit your reflection to receive your AiCE Points certificate.
Take Assessment & Get CertificateLearning Objectives
- •Understanding bruxism pathophysiology and its clinical manifestations
- •Assessment and diagnosis of masseter hypertrophy
- •Evidence-based botulinum toxin dosing for masseter treatment
- •Integration of masseter assessment into routine clinical examinations
- •Patient selection criteria and outcome measurement
This comprehensive review examines bruxism as a global condition affecting approximately 22% of adults, its manifestations including masseter hypertrophy and orofacial pain, and the role of botulinum toxin in treatment. The article details how bruxism leads to muscle hypertrophy, dental damage, and TMJ dysfunction, and provides evidence-based guidance on using Botox injections to reduce bite force, relieve pain, and improve facial aesthetics. The review synthesises current research showing that Botox significantly reduces bite force and pain for 3-4 months, whilst also addressing the aesthetic concerns of masseter hypertrophy.
Introduction
Bruxism is a common parafunctional activity characterised by involuntary, excessive clenching or grinding of the teeth, often accompanied by rhythmic contractions of the jaw muscles. It can occur during sleep (sleep bruxism) or wakefulness (awake bruxism), and both forms are widespread globally. Recent meta-analytic data indicate that roughly one in five adults experiences bruxism: the combined global prevalence is about 22% (sleep bruxism ~21%, awake bruxism ~23%).
Bruxism is often overlooked in general practice, yet it can have significant consequences for oral and facial health. Patients may present with tooth wear (flattening or chipping of teeth), jaw pain, morning temporal headaches, or temporomandibular joint (TMJ) stiffness. In severe or chronic bruxism, the excessive loading of the masticatory muscles (primarily the masseter and temporalis) can lead to muscle hypertrophy and orofacial pain.
Importantly, bruxism has a multifactorial aetiology and is now understood to be at least partly a centrally mediated phenomenon. Sleep bruxism in particular is considered a sleep-related movement disorder tied to micro-arousals of the central nervous system. This central origin explains why traditional peripheral treatments (e.g. mouthguards) may alleviate symptoms and protect the teeth but do not necessarily cure the underlying driver of bruxism.
Pathophysiology of Bruxism
Bruxism is broadly classified into sleep bruxism (SB) and awake bruxism (AB), which differ in their triggers and awareness. Sleep bruxism often occurs during micro-arousals in sleep; the brainstem arousal leads to a rise in autonomic activity and activation of jaw muscles in an unconscious rhythmic pattern. In contrast, awake bruxism is usually semi-voluntary clenching or grinding during daytime, often driven by stress, concentration, or habit.
Over time, this neuromuscular overactivity can cause hypertrophy of the masseter (and sometimes temporalis) muscles, similar to how repetitive exercise enlarges skeletal muscles. Patients with long-standing bruxism often develop visibly enlarged jaw muscles and a stronger bite force. Ultrasonographic and electromyographic studies have confirmed that bruxism is associated with increased masseter muscle thickness and activity.
Orofacial pain in bruxism arises from sustained muscle contraction and joint overload. The constant clenching can lead to myalgia in the jaw muscles – patients often report sore, stiff masseters or tenderness in the temples upon waking. This can manifest as tension-type headaches, especially in the temporal region.
Masseter Muscle Hypertrophy
The masseter muscle is the primary jaw-closing muscle, originating from the zygomatic arch (cheekbone) and inserting at the mandibular angle. With chronic hyperactivity as in bruxism, this muscle can undergo hypertrophy, meaning an increase in bulk and cross-sectional size. Masseter hypertrophy may be unilateral or bilateral, and patients present with a noticeably wider lower face or a more square jawline.

From an aesthetic perspective, masseter hypertrophy can dramatically alter facial shape. An attractive or youthful female face is often described as having a "V-shape" or triangle of youth, where the widest part of the face is at the cheeks and it tapers to a slimmer jaw and chin. Excessive growth of the masseters makes the lower third of the face wider relative to the upper and middle thirds, creating what has been termed "pseudo-ageing".
Clinical Grading System
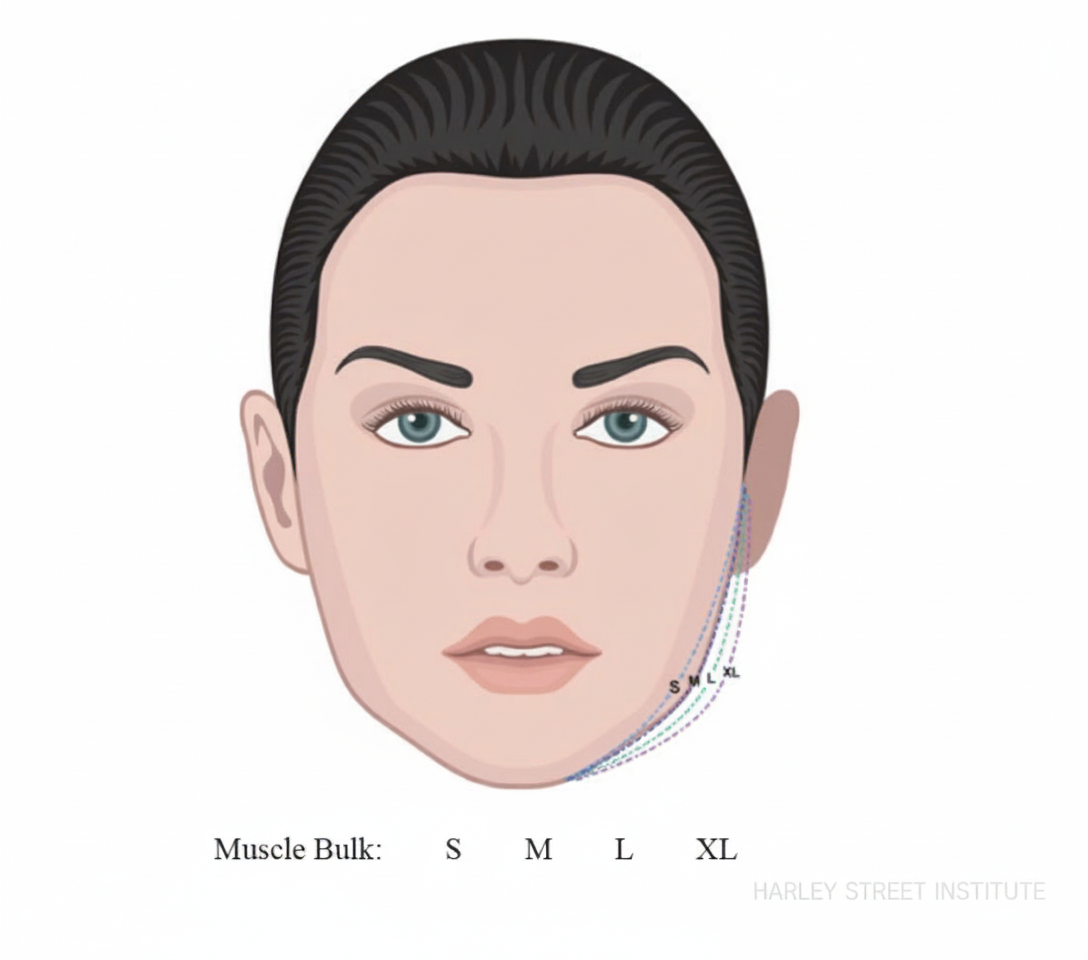
Harley Institute Grading:
- Small (Normal): Lower face clearly narrower than cheekbone width. Graceful oval or heart shape.
- Medium: Jaw approaching width of cheeks. Mild bulge at mandibular angle on clenching.
- Large: Lower face width equals cheekbone width. Masseter visibly thick at rest.
- Extra-Large: Jaw wider than cheekbones. Bottom-heavy face with extremely bulky masseters.
Conventional Management
Managing bruxism often requires a multidisciplinary approach. First-line management is typically conservative:
- Occlusal Splints (Night Guards): Custom-moulded dental appliances that separate teeth, preventing tooth-on-tooth damage.
- Behavioural Modifications: Habit awareness, stress reduction, biofeedback, and jaw relaxation exercises.
- Physical Therapy: Jaw physiotherapy, massage, and stretching exercises.
- Medications: Muscle relaxants, anxiolytics, or clonazepam for refractory cases.
Botulinum Toxin Treatment
Botulinum toxin type A (BoNT-A) has emerged as a promising treatment for bruxism. It acts by blocking acetylcholine release at the neuromuscular junction, causing temporary chemodenervation of muscle fibres. When injected into hyperactive muscles like the masseter, it results in partial paralysis, reducing contraction force.
Therapeutic Benefits
By diminishing masseter strength, botulinum toxin can break the cycle of clenching and muscle pain. A systematic review and meta-analysis (2023) found that Botox injections led to significant reduction in bite force as early as 1 month compared to placebo. Pain severity also decreased more in Botox-treated patients, with a dose-dependent effect.
Benefits typically appear within 2-4 weeks, peak around 6-8 weeks, and last up to 3-4 months before diminishing. This aligns with the known duration of action of BoNT-A in muscle.
Aesthetic Benefits
From a cosmetic standpoint, Botox in the masseters is a well-established treatment to slim the jawline. By causing atrophy of an enlarged masseter, the lower face can become noticeably narrower. Within 2-4 weeks post-injection, patients begin to see a softer jaw contour; by 6-8 weeks the maximal reduction in muscle volume is apparent.
Studies have shown an average cross-sectional area reduction of ~30% after a single injection, with further enhancement after repeat treatments.
Dosage and Technique
Masseter Injections:
Typical starting dose: 20–30 units of onabotulinumtoxinA per masseter for average adult with significant bruxism or hypertrophy.
Dose adjustments: Males or very large muscles may require 40–50+ units per side; females with moderate hypertrophy might do well with ~20 units/side.
Injection Points
The masseter is usually injected at 2–3 points: one in the belly of the superficial masseter (near prominence when teeth clenched), and one or two more along the lower border of the mandible. Some practitioners use a four- or six-point grid for very large muscles.
Temporalis Injections
For cases with significant temporalis involvement (temporal headaches or large temporalis muscles), doses of 10–20 units per temporalis (divided into 2–3 sites) have been used.
Safety and Side Effects
When administered by a trained professional, botulinum toxin injections are generally safe. Common side effects are usually localised and temporary:
- Mild pain or bruising at injection site
- Transient weakness in chewing (expected treatment effect)
- Rare asymmetry or smile changes if toxin diffuses to nearby muscles
- Slight change in bite feel as muscle atrophies
Conclusion
Bruxism is a prevalent and multifaceted condition affecting a broad swath of the population globally. For front-line healthcare providers, recognising bruxism and its manifestations is crucial. Unexplained dental wear, jaw pain, headaches, or hypertrophic jaw muscles should prompt evaluation for bruxism and related TMJ disorders.
Management traditionally centres on conservative measures like splints and behavioural therapy, which remain important. However, the advent of botulinum toxin injections has added a powerful tool to the bruxism treatment arsenal, especially for patients with muscle hypertrophy or chronic myofascial pain. Research shows it significantly reduces bite force and pain for up to 3-4 months, and patients can experience improved quality of life as a result.
From an anatomic and pathophysiological standpoint, understanding the role of the masseter and temporalis in bruxism guides us to targeted therapies. Masseter hypertrophy is not merely a cosmetic concern but a marker of chronic jaw overload. Addressing it can solve medical complaints whilst simultaneously enhancing facial aesthetics – a win-win scenario for patients.
In conclusion, modern treatment modalities such as botulinum toxin injections have revolutionised management of bruxism and related conditions, providing relief and cosmetic enhancement with minimal invasiveness. With timely intervention, patients can be spared the long-term damage of bruxism and enjoy not just improved oral health, but often a refreshed, more youthful facial appearance as well.
Key References
1. Zieliński G, et al. Global Prevalence of Sleep Bruxism and Awake Bruxism: A Systematic Review and Meta-Analysis. J Clin Med. 2024;13(14):4259.
2. Chen Y, et al. Effectiveness of Botulinum Toxin Injection on Bruxism: A Systematic Review and Meta-analysis. Aesthetic Plast Surg. 2023;47(2):775-790.
3. Nobre BBS, et al. Exploring botulinum toxin's impact on masseter hypertrophy: a randomised trial. Sci Rep. 2024;14:14522.
4. De la Torre Canales G, et al. Botulinum toxin in the management of masticatory myofascial pain. J Oral Rehabil. 2022.
5. Lee HJ, et al. Repeated botulinum toxin injections into masseter induce bony changes: A longitudinal study. Korean J Orthod. 2017;47(4):222-228.
Related Training at Harley Street Institute
This article was generated by HSI AI and represents a synthesis of current medical literature on bruxism and botulinum toxin treatment.
