Skin Repair Mechanisms
Controlling inflammation and restoring barrier integrity
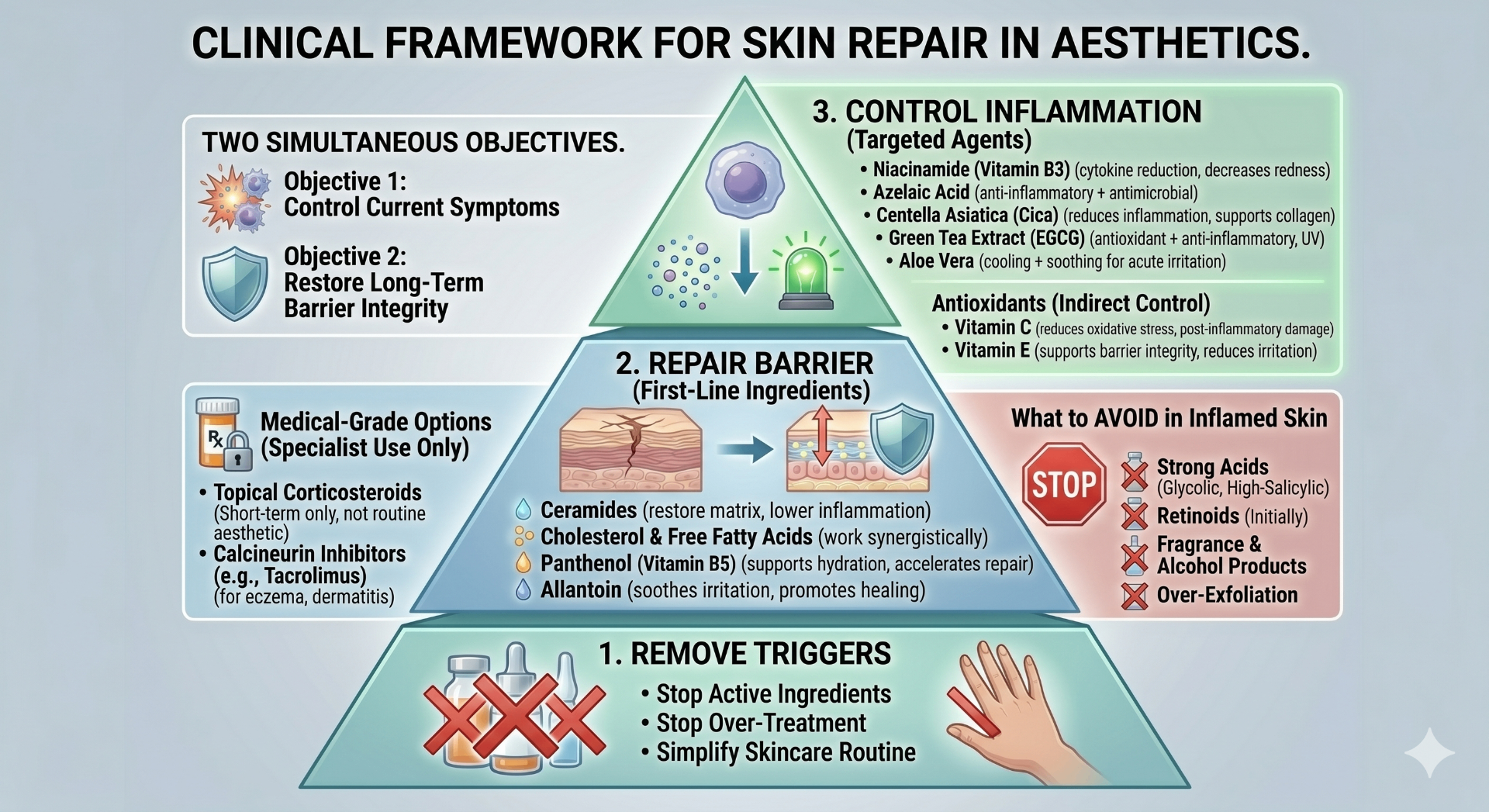
Skin repair in aesthetic practice has two distinct objectives that must be addressed simultaneously:
- Objective 1: Control current symptoms — reduce redness, stinging, and reactivity now
- Objective 2: Restore long-term barrier integrity — so these problems do not return
When skin is inflamed, the immediate priority is to remove triggers. Stop active ingredients, stop over-treatment, and simplify the skincare routine. This alone can reduce inflammatory load significantly.
Barrier-Repair Ingredients (First-Line)
The lipid matrix of the stratum corneum must be restored before anything else:
- Ceramides — restore the lipid matrix, reduce TEWL, indirectly lower inflammation
- Cholesterol + Free Fatty Acids — work synergistically with ceramides to improve barrier integrity
- Panthenol (Pro-vitamin B5) — supports hydration and accelerates repair
- Allantoin — soothes irritation and promotes healing
Direct Anti-Inflammatory Agents
Once the barrier is stabilising, introduce targeted anti-inflammatory ingredients:
- Niacinamide (Vitamin B3) — reduces inflammatory cytokines, improves barrier function, decreases redness
- Azelaic Acid — anti-inflammatory + antimicrobial, effective for erythema, acne, rosacea, and PIH
- Centella Asiatica (Cica) — reduces inflammation, promotes wound healing, supports collagen
- Green Tea Extract (EGCG) — antioxidant + anti-inflammatory, reduces UV-induced inflammation
- Aloe Vera — cooling + soothing for acute irritation
Antioxidants (Indirect Inflammation Control)
- Vitamin C — reduces oxidative stress, helps post-inflammatory damage
- Vitamin E — supports barrier integrity, reduces irritation
What to AVOID in Inflamed Skin
- Strong acids — glycolic, high-percentage salicylic
- Retinoids — initially, until barrier is restored
- Fragrance and alcohol-heavy products
- Any form of over-exfoliation
Medical-Grade Options (Specialist Use Only)
- Topical Corticosteroids — strong anti-inflammatory, short-term use only, not routine aesthetic use
- Calcineurin Inhibitors (e.g., Tacrolimus) — reduce immune activation in eczema and dermatitis
The 3-Step Clinical Framework
This must be followed in order:
- Step 1: Remove Triggers — stop actives, stop over-treatment
- Step 2: Repair Barrier — ceramides, panthenol, gentle moisturisers
- Step 3: Control Inflammation — niacinamide, azelaic acid, soothing botanicals
Treatment Modalities — A Structured Overview
Finally, a structured overview of the treatment modalities discussed. The clinical 4-quadrant framework presents photo-realistic vignettes of each option: CHEMICAL PEELS (cool blue) for controlled exfoliation and pigment turnover; LASER / IPL (pulsed red) for targeted vascular and melanocytic correction; MICRONEEDLING (gentle green) for barrier remodelling and collagen induction; and TOPICAL THERAPIES (soft amber) for daily inflammation, barrier, and melanocyte support. Selecting the right modality for the right condition is an analytical decision — not a technique. Each quadrant maps onto the underlying drivers (Inflammation, Barrier, Melanocytes), reinforcing that modality choice must follow diagnosis, not preference.
Clinical Takeaway
You don't treat inflammation with stronger treatments — you treat it by restoring control. Remove triggers, repair the barrier, then control inflammation.
Frequently Asked Questions
What are the best ingredients for controlling skin inflammation?
Niacinamide (Vitamin B3) reduces inflammatory cytokines and improves barrier function. Azelaic acid is effective for erythema and pigmentation. Ceramides restore the lipid matrix. Centella Asiatica and green tea extract provide botanical anti-inflammatory support. These should be introduced after triggers are removed and barrier repair has begun.
What should I avoid on inflamed skin?
Avoid strong acids (glycolic, high-percentage salicylic), retinoids (initially), fragrance and alcohol-heavy products, and over-exfoliation. These will further disrupt the barrier and amplify inflammation.
What is the 3-step clinical framework for inflamed skin?
Step 1: Remove triggers — stop actives and over-treatment. Step 2: Repair barrier — use ceramides, panthenol, and gentle moisturisers. Step 3: Control inflammation — introduce niacinamide, azelaic acid, and soothing botanicals. This sequence must be followed in order.
Key Points
- Two goals: control current symptoms and improve long-term barrier integrity
- Ceramides, cholesterol, and fatty acids restore the lipid matrix
- Niacinamide and azelaic acid are first-line anti-inflammatory agents
- Avoid strong acids, retinoids, and fragrance on inflamed skin
- Follow the 3-step framework: Remove Triggers → Repair Barrier → Control Inflammation
Clinical Tip
When a patient presents with inflamed, reactive skin — simplify everything first. The most powerful intervention is often subtraction, not addition.
Continue Your Clinical Dermatology Training
This page is part of the CAD – Certificate in Aesthetic Dermatology by Harley Street Institute. Unlock the full structured programme to build clinical confidence in dermatological assessment.
