Sensitized Skin
Triggers, chronic inflammation & mediators
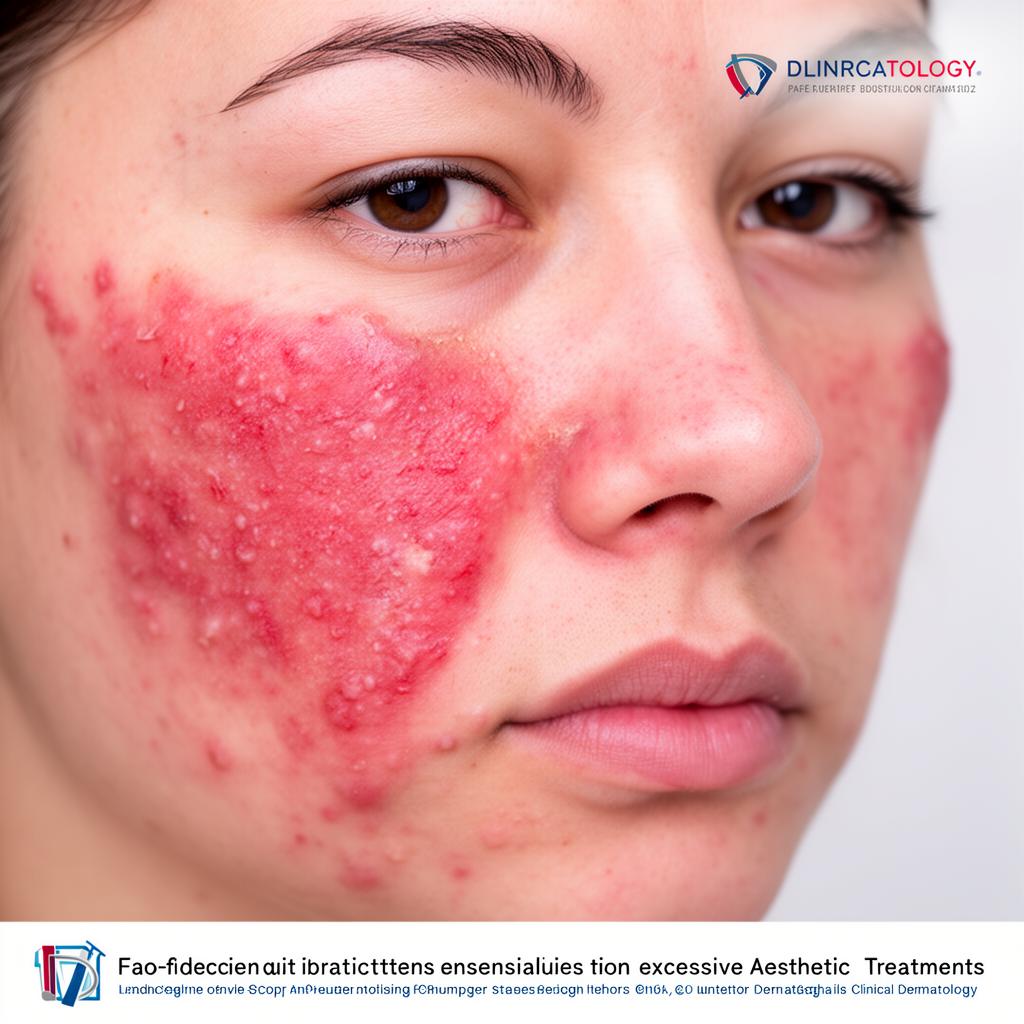
Sensitized skin is different from sensitive skin. It is an acquired condition — meaning it develops over time in response to specific triggers. Understanding what causes sensitization, and the inflammatory processes that sustain it, is essential for safe aesthetic practice.
The most common triggers of skin sensitization include:
- Skincare products — overuse of retinoids, AHAs, BHAs, vitamin C at high concentrations, and products with fragrance, alcohol, or essential oils. Layering multiple active ingredients without adequate barrier support is one of the most frequent causes seen in aesthetic patients.
- Previous skin conditions — patients with a history of acne, eczema, or psoriasis often have a compromised barrier that makes them more susceptible to sensitization. The skin may appear "normal" but remains structurally vulnerable.
- Contact dermatitis — both irritant and allergic contact dermatitis can trigger sensitization. Repeated exposure to irritants (cleansers, preservatives, latex) or allergens gradually weakens the barrier and primes the immune system for overreaction.
- Aggressive aesthetic treatments — frequent chemical peels, over-exfoliation, microneedling without adequate recovery, and laser treatments performed too close together can all push the skin into a sensitized state.
- Environmental factors — chronic UV exposure, pollution, and extreme climate changes contribute to ongoing barrier stress.
When these triggers persist, the result is chronic, low-grade inflammation. Unlike acute inflammation — which is a healthy, time-limited healing response — chronic inflammation is sustained, self-perpetuating, and damaging. The skin remains in a constant state of low-level immune activation.
This chronic inflammation is driven by specific mediators — signalling molecules released by damaged cells and immune cells in the skin:
- Cytokines (IL-1, IL-6, TNF-α) — these are pro-inflammatory proteins released by keratinocytes and immune cells in response to barrier damage. They amplify the inflammatory response and recruit more immune cells to the area, creating a cycle of ongoing inflammation.
- Prostaglandins — lipid compounds produced at the site of tissue damage. They cause vasodilation (redness), increase permeability (swelling), and heighten pain sensitivity (stinging and burning sensations that sensitized patients report).
- Histamine — released by mast cells in the dermis. It causes itching, redness, and increased vascular permeability. Patients with sensitized skin often have elevated mast cell activity.
- Reactive Oxygen Species (ROS) — free radicals generated by UV exposure, pollution, and cellular stress. They damage cell membranes and lipids, further weakening the barrier and sustaining the inflammatory cycle.
This is why sensitized skin cannot be treated with more stimulation. The inflammatory mediators are already elevated. Adding peels, actives, or devices simply amplifies the cycle. The solution is to reduce the triggers, calm the mediators, and allow the barrier to recover.
Patients may report that their skin has become "worse" over time despite ongoing treatments. This is the hallmark of sensitization — the treatments themselves are sustaining the problem.
Many patients do not need more intervention — they need recovery.
Clinical Takeaway
Sensitization is driven by chronic, low-grade inflammation. You cannot treat sensitized skin with more stimulation — you must first resolve the inflammatory cycle.
Frequently Asked Questions
What triggers skin sensitization?
Common triggers include overuse of active skincare ingredients (retinoids, AHAs), previous skin conditions like acne or eczema, contact dermatitis from irritants or allergens, aggressive aesthetic treatments, and chronic environmental exposure.
What is the role of cytokines in sensitized skin?
Cytokines such as IL-1, IL-6, and TNF-α are pro-inflammatory proteins released by damaged keratinocytes and immune cells. They amplify inflammation and recruit more immune cells, creating a self-perpetuating cycle of barrier damage and reactivity.
Why does sensitized skin get worse with more treatment?
Because the inflammatory mediators (cytokines, prostaglandins, histamine, ROS) are already elevated. Additional treatments amplify these signals rather than resolving them. The skin needs reduced stimulation and barrier repair, not more active intervention.
How do you treat sensitized skin?
Reduce triggers (simplify skincare, pause active treatments), calm inflammation, and focus on barrier repair with gentle, pH-balanced products. Allow adequate recovery time — typically 4-8 weeks — before reintroducing any actives.
Key Points
- Key triggers: products, acne history, contact dermatitis, over-treatment, UV
- Chronic inflammation is sustained by cytokines, prostaglandins, histamine, and ROS
- Inflammatory mediators amplify the damage cycle — more treatment makes it worse
- The solution is to reduce triggers and allow barrier recovery
Clinical Tip
If a patient reports progressive worsening despite regular treatments, consider sensitization. Ask about their full skincare routine, treatment history, and any history of acne, eczema, or contact dermatitis.
Continue Your Clinical Dermatology Training
This page is part of the CAD – Certificate in Aesthetic Dermatology by Harley Street Institute. Unlock the full structured programme to build clinical confidence in dermatological assessment.
